At National Health Foundation (NHF), we believe that a hospital discharge should represent a successful transition to the next stage of recovery, especially for those experiencing homelessness. Through CalAIM, recuperative care, also known as medical respite, has emerged as a vital “Community Support,” acting as a bridge between a hospital bed and a more stable future.
To ensure this model works as effectively as possible, it is important to look at how we structure the Length of Stay (LOS) for participants. While policy discussions often explore the use of global caps or time-bound limits, our goal as a service provider is to ensure that care remains tailored to individual needs.
Our latest analysis of NHF’s 2024 program data provides helpful insights into how the duration of care impacts a participant’s journey. The data suggests a clear trend: providing recuperative care guests with sufficient time to recover leads to stronger outcomes.
What the Data Tells Us
To understand how time impacts recovery, we tracked participant progress using the Housing Path Score (HPS), an internal metric for housing readiness. We looked at three groups: those staying less than 30 days, 30–60 days, and 60–90 days.
The findings were definitive:
• Progress is Universal: Across all categories, participants demonstrated measurable improvement in their HPS during their stay.
• Time Matters: Both the magnitude and the probability of improved scores increased significantly with longer stays.
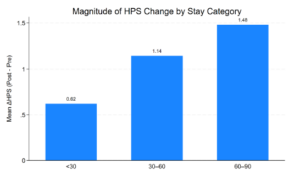
• Maximum Gains: Participants in the 60–90 day category experienced the largest average gains in their HPS.
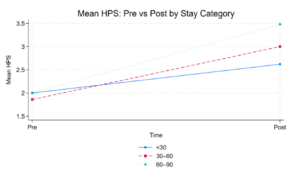
• The 30-Day Window: While those staying 30 days or less also showed improvement, the gains were smaller on average, reflecting the limited time available for medical stabilization and discharge planning. (See images below for graphs of Magnitude of HPS Change and Mean HPS change over time.)
The Importance of Flexibility
Recuperative care is most effective when it is treated as a clinical transition rather than a standardized, time-limited service. When stay durations are flexible, the program can better fulfill its core functions by providing enough time for thorough medical stabilization and care coordination. These adequate stays protect the broader health system by preventing premature discharges, which reduces the risk of avoidable hospital readmissions and helps lower total system costs. Ultimately, maintaining flexibility allows providers to use their discretion to determine when a participant is truly ready for a safe discharge, ensuring the service functions as intended under CalAIM.
A Path Forward for Policy
For recuperative care to function as intended under CalAIM, policy design should align with these observed outcome patterns. Based on our findings, NHF suggests the following:
1. Avoid rigid caps that may unintentionally interrupt the recovery process.
2. We recommend proposing policies, similar to AB 804, that would make recuperative care a guaranteed Medi-Cal benefit.
3. Protecting LOS flexibility supports both participant well-being and the long-term efficiency of the health system.
Healing is a process that requires both care and time. By ensuring our policies reflect the reality of medical recovery, we can help the most vulnerable members of our community achieve lasting health and housing stability.
To dive deeper into the housing outcomes of our recuperative care guests, we plan on moving on to phase 2 of this study in mid-2026. Phase 2 will include adding additional guests LOS to the analysis (n = 150), looking at outcomes for guests who stay longer than a 90-day period, including guests from our newest site (Arleta), and including Coordinated Entry Scores (CES) as a data point for analysis. For more information on NHF’s recuperative care program, check here: https://nationalhealthfoundation.org/recuperative-care/program-services/ and to learn more about this LOS analysis, please reach out to cmonk@nhfca.org.
